I’m interested in...
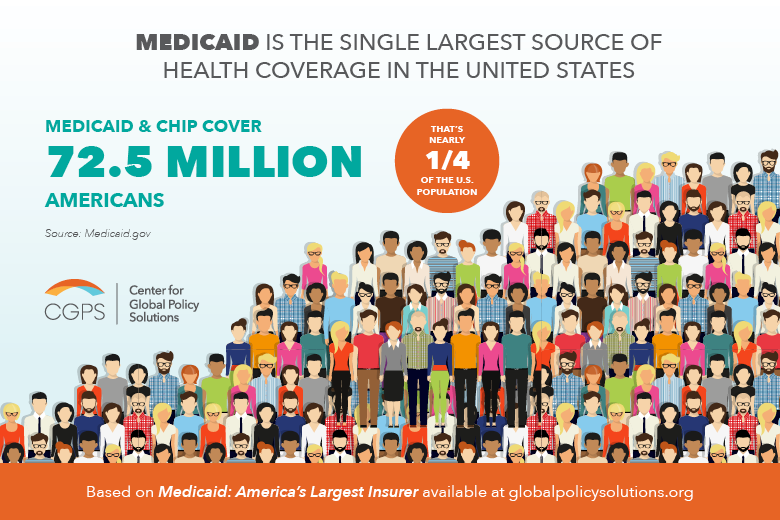
Benefit Management
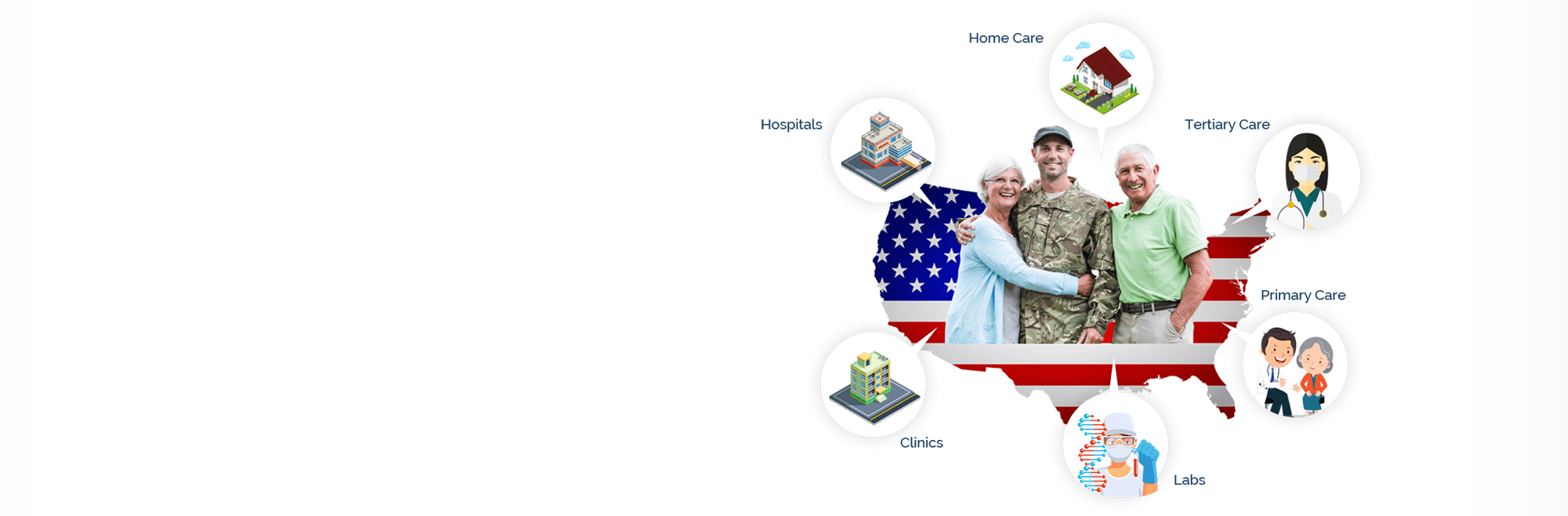
eSimplicity helps federal, state, and local agencies implement public benefits programs with the beneficiary experience in mind. From eligibility determination and enrollment to case follow-up and payments, we design solutions with a human-centered design (HCD) approach that puts the user first. This helps the American public sift through a lot of information from the web, the community, the service broker, and federal and state agencies as they search, identify, and enroll in needed services.
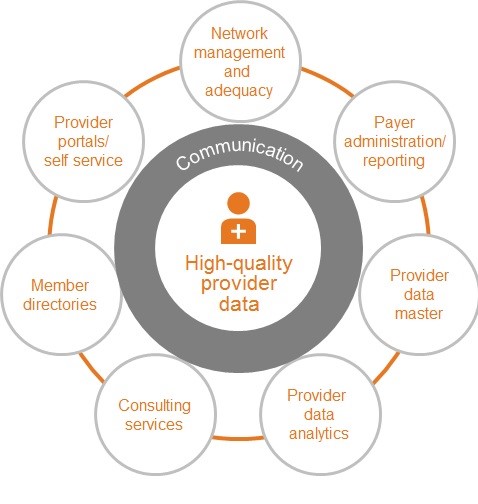
Provider/Supplier Management
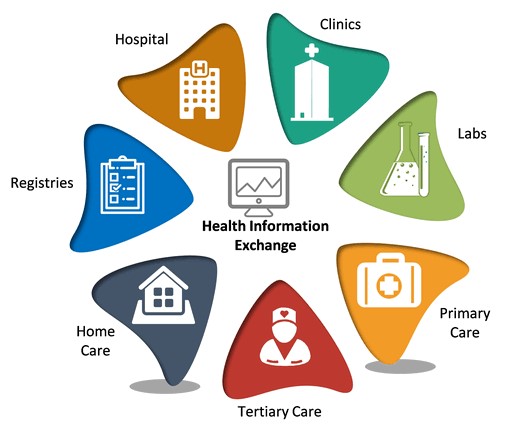
Public benefits programs often have many providers and suppliers that deliver services or products to beneficiaries. eSimplicity develops tools that support collaborative efforts between government agencies and providers. Our healthcare quality portal allows tens of thousands of providers to register their organization, receive new information related to their programs, submit healthcare quality measurement data, and exchange data with the government. We also support the government in implementing business intelligence reports on provider risk scores in support of the program’s integrity effort.

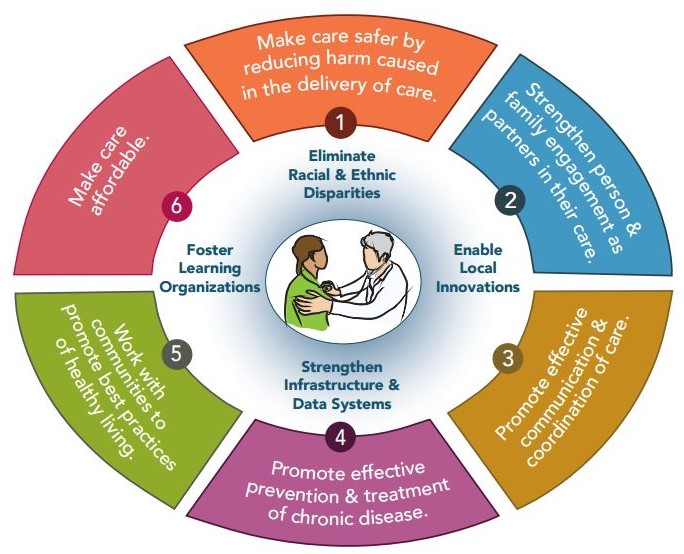
Social Services and Case Management
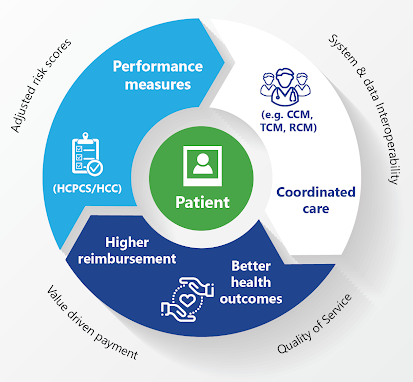
Robust case management systems present and deliver data from various sources to case workers. eSimplicity uses a low-code approach with cloud based computing solutions (e.g., Salesforce and Appian) to facilitate process workflow, allowing states and the federal government to collaborate on plans for groups of covered individuals, provide services, reimburse providers, and perform administrative activities at the state level. eSimplicity’s low-code Identity Governance as a Service (e.g., Saviynt) implementation solution is used by CMS providers and trading partners to securely exchange data for identity management and role-based authorization.

Eligibility and Entitlement
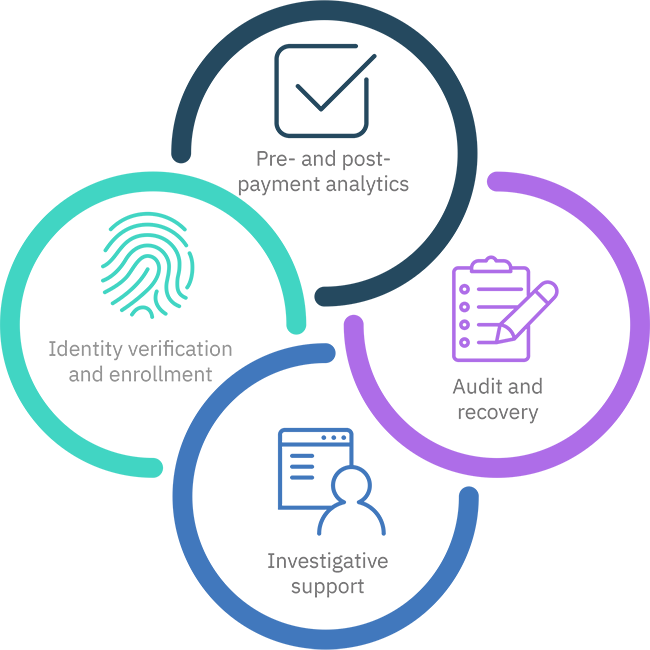
Eligibility and entitlement information must be verified for many public benefits programs before services are rendered. Beginning with the initial development effort and the subsequent launch in 2014 of the health insurance marketplace (www.healthcare.gov), eSimplicity’s team supports the implementation of complex eligibility and entitlement criteria that spans many federal and state data sources and continuously analyzes website data and user behaviors. eSimplicity modernizes legacy beneficiary and eligibility systems that allow downstream systems and programs to obtain real-time eligibility information; moves eligibility and entitlement information and its API to the cloud to streamline operations and lower maintenance cost; and uses real-time integration with a data service hub so the CMS team can accelerate the eligibility determination process, reduce errors, and elevate user experience.
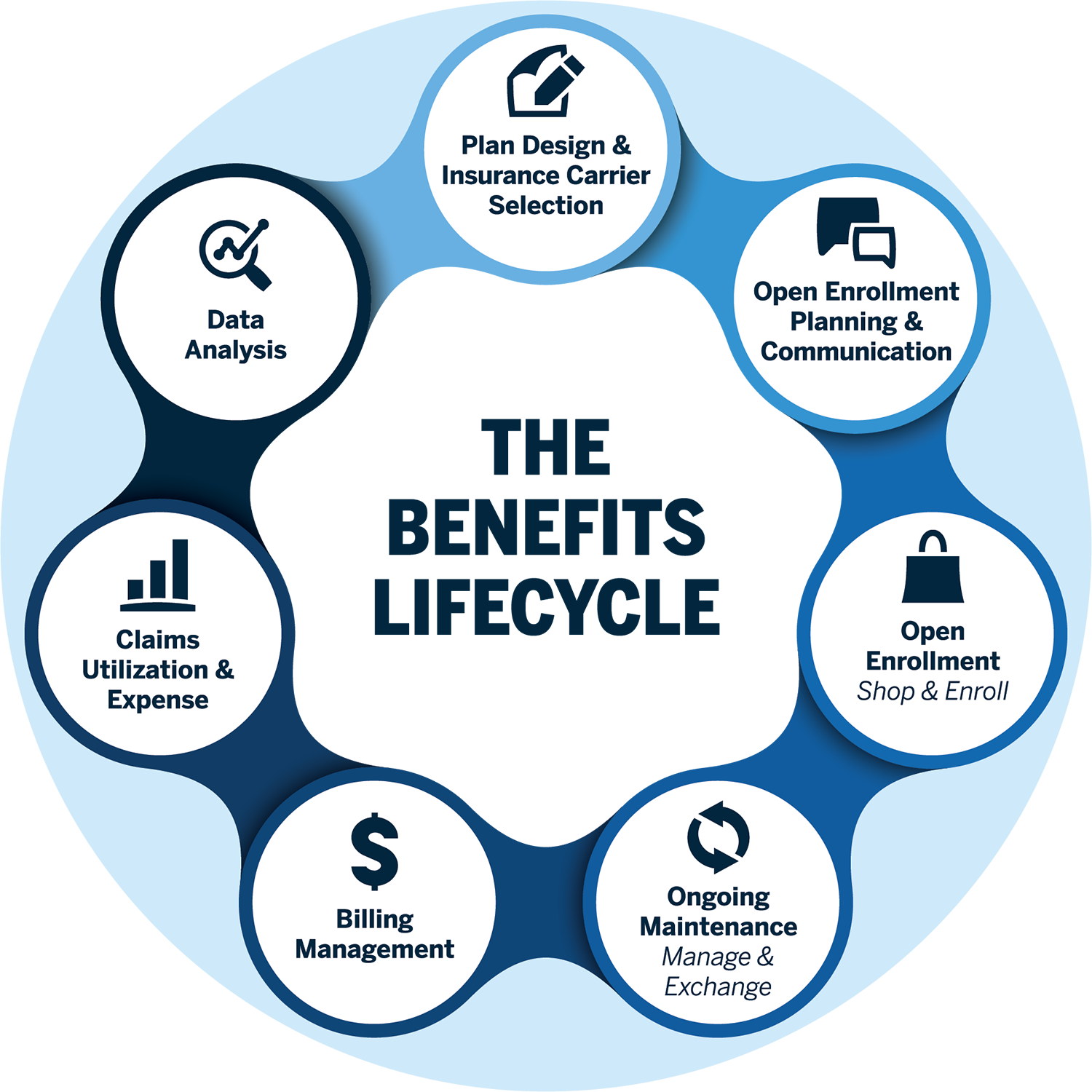
Enrollment and Payment
To reach the greatest number of enrollees, public benefits programs implement multiple enrollment methods and outreach activities. eSimplicity’s team supports the federal insurance marketplace, which offers enrollment via a direct online enrollment website, agent brokers, call centers, and other means. Our insurance specialists verify the complex enrollment workflow and payment aggregation process that integrates various federal and state services. We focus on the user experience and data integrity for enrollees, health plan issuers, agent brokers, and the CMS and state users.