Challenge
Each year millions of Americans request healthcare coverage through the healthcare.gov website. From eligibility rules, coverage options, complex drug benefits to provider network selection and potential hidden benefits, many individuals have to learn through insurance broker agents or search for the information on the healthcare.gov website themselves.
Solution
For the CMS, our engineers support multiple modules within the Federally Facilitated Marketplace (FFM) to ensure individuals have a great user experience and accurate results in terms of eligibility and enrollment. eSimplicity insurance specialists and performance engineers work with the integrated marketplace team to continually release new applications, APIs, and functions to improve both the end user experience, promote interoperability with brokers, and reduce burdens on the plans.
Outcomes
Millions successfully enrolled in the right plans for them and their families every year. Their experience browsing and enrolling in a health plan has been improved significantly this year. Users can now stay on the same broker’s website and complete their entire transaction – made possible by the team delivering the APIs to the web brokers.
Expanding healthcare coverage to millions. It’s a great call in helping many Americans who need it most by obtaining a healthcare insurance plan that works for their needs, regardless of a pre-existing condition. eSimplicity insurance specialists, performance engineers, and data analysts work to validate and test application and data to simplify the insurance selection and purchase. Moreover, our risk adjustment data analysts help analyze risk adjustment data to help stabilize premiums and offer a variety of plans for individuals with different health care needs, sustaining the marketplace healthcare coverage expansion model.
Areas of Expertise


Data Service Hub
Data Services was created by the Internal Revenue Service (IRS) and Health and Human Services (HHS). The hub transmits and verifies the individual’s income and tax data from IRS records, SSN info from Social Security Administration, Immigration information from Homeland Security, and USCIS and multiple other data sources from the federal agencies including the Department of Defense, the Department of Veterans Affairs, the Office of Personnel Management, the Peace Corps, and state Medicaid administrations. eSimplicity engineers work to validate these hub services are updated according to policy changes.
Eligibility
The eligibility determination ensures that consumers receive accurate eligibility determination based on family size and relationship, income (FPL level) and previous coverage (if any), and grants the correct amount on Annual Premium Tax Credit (APTC) for consumers or refers them to Medicaid/CHIP per the state agency determination laws. Eligibility standalone services are created and accessible to marketplace issuers through APIs which allows for customization of the application process within the federal guidelines.
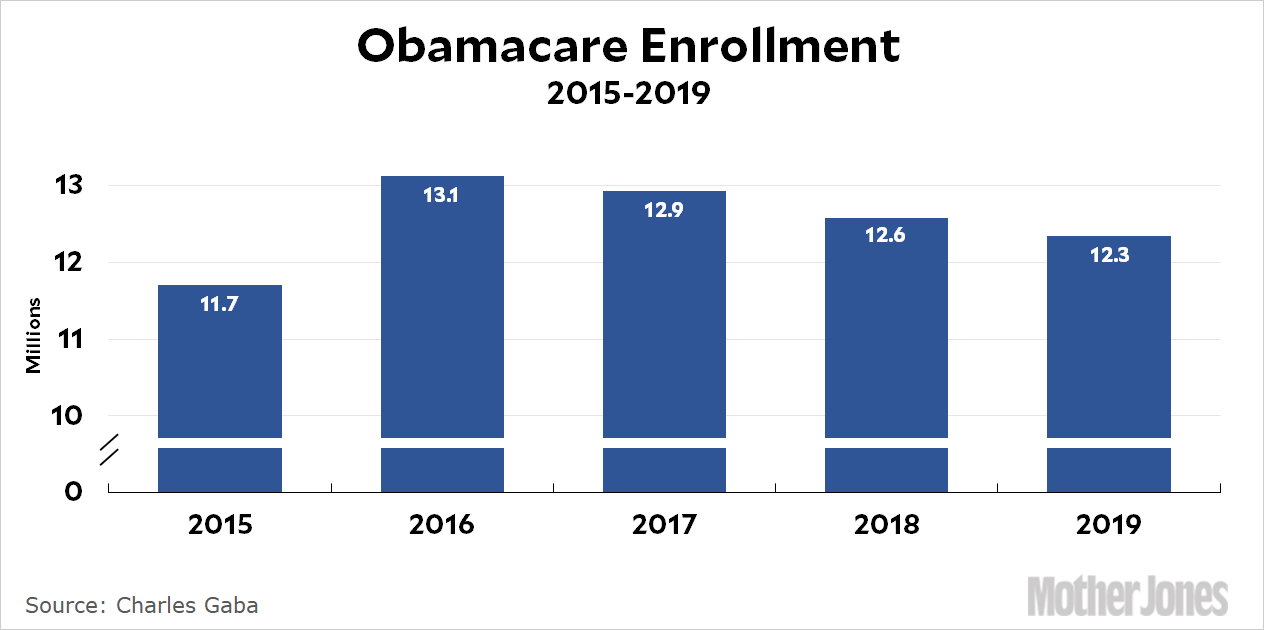
Enrollment
The Enrollment Processing module maintains a consolidated data store that contains both FFM and state-based marketplace (SBM) enrollment records to allow for accurate payments to be remitted to the issuers. The module processes enrollment transactions from both FFM and SBMs.
Payment Processing
In order to make payments and pursue collections to and from issuers and other entities, CMS needs to process user fees, reinsurance, risk adjustments, and risk corridors payment (and charge) amounts, aggregate them and send to the ledger system for processing and reconciling these payments with issuers.
Risk Adjustment
The Risk Adjustment (RA) program helps to better spread the financial risk by health insurance Issuers in the individual and small group markets. This stabilizes premiums and provides issuers with the ability to offer a variety of plans to meet the needs of a diverse population. Under the RA program, payments are transferred from Issuers with relatively lower-risk populations to issuers with relatively higher-risk populations.
In addition, a Risk Adjustment User Fee is assessed to each participating issuer to fund the cost of operating the program. Reinsurance provides payments to issuers that incur high costs for claims in individual plans, both inside and outside the market. In accordance with the final rule, reinsurance payments are based on a coinsurance rate or proportion of an issuer’s claims costs that are above an attachment point and below a reinsurance cap for the applicable benefit year.
Plan Compare
The objective is to ensure there are enough plans available geographically to enable consumers to receive the best health plan for their needs. Also, issuers require an ability to ensure that any changes to plans are immediately updated to the marketplace platform so consumers can compare the plans and benefits across various issuers. The PC2.0 platform ensures a smooth transition from the eligibility platform to plan selection for a unified consumer experience.

