Fighting fraud. Most physicians, providers, and suppliers who serve Medicare beneficiaries are committed to providing high-quality care to their patients and to billing the program only for the payments they have earned. Unfortunately, there are also individuals who abuse or defraud Medicare, cheat the program, and in some cases, leave individuals with Medicare liable for co-payments for services never received. Medicare fraud also results in Medicare beneficiaries paying higher premiums. To fight fraud, waste, and abuse, government agencies and contractors need to stay ahead of the fraud schemes while working to not impact or burden honest providers or suppliers that are serving Medicare beneficiaries. eSimplicity is part of a large integrated team helping the government on this effort.
Challenge
Medicare fraud costs tens of billions each year and results in higher health care costs and taxes for everyone. The Centers for Medicare & Medicaid Services (CMS) is always seeking new methods and technologies to prevent fraud, waste and abuse.
Solution
The CMS has multiple programs and companies support the fraud prevention efforts. eSimplicity helps large prime contractors at the CMS implement modern data pipelines that integrate claims, provider, beneficiary and other supplemental data from legacy mainframe and cloud-based data sources to support machine learning capabilities and detect anomalies in claims prior to payment.
Outcomes
The solutions provide a range of benefits, including improved return on investment from administrative actions, improved prevention and detection of fraud, waste, and abuse in Medicare, and cost savings in operational IT infrastructures
Areas of Expertise
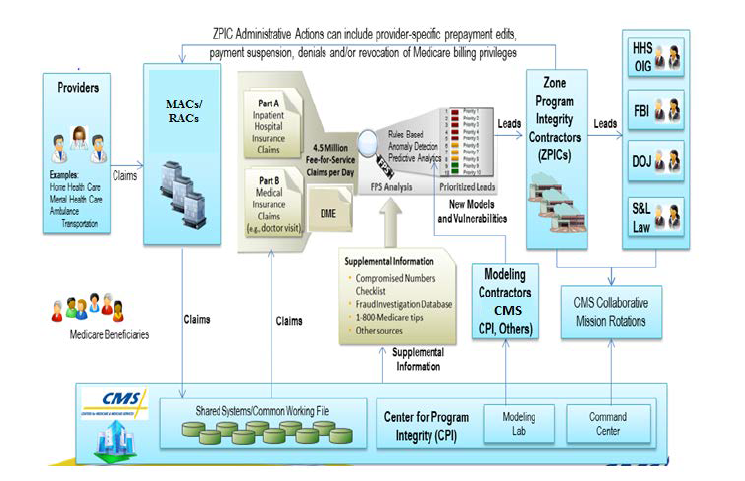
Data Pipeline and Predictive Analytics
The system captures and detects patterns or anomalies through development of provider and beneficiary profiles, identifying potential fraud, waste and abuse by the methods listed below on 4.5 million claims per day for Medicare Part A, Part B and durable medical equipment (DME):
• Provider billing patterns
• Beneficiary utilization patterns
• Use of social network analysis and neural network analysis
• Regression analysis and other approved methods by CMS
The system for risk identification is grounded in sound analytic methodologies and relies on algorithms informed by analytic, medical, clinical, and administrative knowledge that enables identification of improper payments before final payment is authorized by CMS.
